I was worried that without the transplant, she wouldn’t be around to tell her story today. For a month of healing, I kept my friend around in the world, and I would do it all again in a heartbeat.
Friend/donor Erika
My name is Erika, and ten years ago I donated one of my kidneys to Mika.
The first thing I tell people about organ donation is that you don’t have to be a superhero to do it – but besides giving blood, it is one of the easiest ways you can save a life. In fact, after the first year or so, you probably won’t think about it that much.
Why did I become a donor in the first place? I doubt that having surgery for someone else would be anyone’s first choice, but I was close to Mika and knew her medical situation well. She was on dialysis, but having a working kidney would let her live a much longer, healthier life without being tied to a machine for hours each day, and I wanted that for her. Honestly, I waited to see if someone else would step up first, but after some time passed, I raised my hand.
A lot of people will go through a surgery or two in their lives, and I’ve had a couple others myself, so I can tell you that the kidney donation and recovery process will probably be very similar. The differences that stood out to me were the extra tests to make sure I was healthy (not just in the kidneys) and that I would continue to be after donation, and a lot of patient education and questions to make sure that I understood the risks and benefits of donation. I never felt hurried or pressured – in fact, I had to reassure the transplant team that I understood what I was getting into as a young (22-year-old) donor – and the process took several months.
The surgery took place in Iowa City, a couple hours away from where we lived, during my college summer break. My dad and I arrived at the hospital early in the morning. I was given an anti-anxiety drug before being wheeled into the operating room, and I remember being fascinated with the equipment there before I went under general anesthesia for a few hours. The next thing I knew, I was in a recovery room, then in my own hospital bed, and I was woozy and sore but told that the surgery went great.
The first 24 hours after the surgery were the hardest, because I felt nauseous and weak, but was told to get up and walk every few hours. I wobbled down the hall to see Mika, who seemed to be feeling better than before, despite the surgery, because she had a working kidney again. She ate a hamburger when I was still trying to keep down simple foods! I spent most of the rest of my time trying to sleep and watching TV until I was discharged after two days and my dad drove us home.
The first few days at home, my routine consisted mainly of sleeping in a recliner, watching Star Trek reruns, getting up to use the bathroom, then needing to rest again. My parents were my main support during that time, and any donor will need a caregiver for the first couple of weeks to do things like cook, help you to doctor’s appointments, and pick up the remote when it falls from your chair – no bending or lifting anything remotely heavy. Things improved slowly but steadily, except for a minor infection at one incision site and a hematoma (a pocket of blood) that I had to go back to Iowa City to have drained when it didn’t go away on its own – the latter was a painful but rare complication that set me back for a while. Working from home wasn’t an option for me at the time, but I probably could have resumed that after two weeks, and I was out and about after a month.
And honestly, that was it. Once the incisions healed and my body felt like it was at full strength again, I resumed my normal life, aside from friends at parties thinking that donating a kidney meant that I wasn’t supposed to be drinking alcohol anymore. The only things that remind me of the surgery now are talking to Mika, seeing the scars when I undress, having a few extra tests at my annual checkups, and taking Tylenol instead of Advil or aspirin – I can still take NSAID painkillers in a pinch, but I should avoid them for the sake of the remaining kidney. Being a donor hasn’t made me ineligible for any other activity or medical procedure.
In the meantime, I know that Mika has been much healthier and able to get more out of life because of my kidney. Kidneys help your body in ways that dialysis can’t, and she’s been able to live and go places more independently without needing to be near a dialysis machine. Because of her rare disease, cystinosis, I knew that her new kidney would gradually lose function, but I also decided early on that the long stretch of time in between our transplant and possibly her next one would be worth it. I was worried that without the transplant, she wouldn’t be around to tell her story today. For a month of healing, I kept my friend around in the world, and I would do it all again in a heartbeat.
Information on Living Donation
There are two main types of living donation:
Directed donation – This is when the donor names a specific person who will receive the kidney
Nondirected donation – This is when a donor does not name a specific person who will get the kidney.
The “full evaluation”
Financial consultation – Transplant center staff will ask about your finances and insurance coverage.
Psychological evaluation – The transplant team will make sure that you are in good mental health and understand the donation process.
Medical tests –
- Medical history: asks for your complete and thorough history of any illnesses, surgeries, and treatments
- Physical exam: physical examination
- Chest X-ray and electrocardiogram (EKG): check for heart or lung disease.
- Radiological testing: looks at your kidney and its blood vessel supply.
- Urine testing: 24-hour urine sample is collected to measure kidney function.
- Gynecological examination: may need to be performed
- Cancer screening: may include colonoscopy, prostate exam, and skin checks
- Compatibility tests: blood sample that includes:
- Blood typing: blood type will be checked
- Tissue typing: checks tissue match between your white blood cells and the recipient’s white blood cells
- Crossmatching: A “positive” crossmatch means that your organ will not match the recipient. A “negative” crossmatch means that your organ is compatible with the recipient.
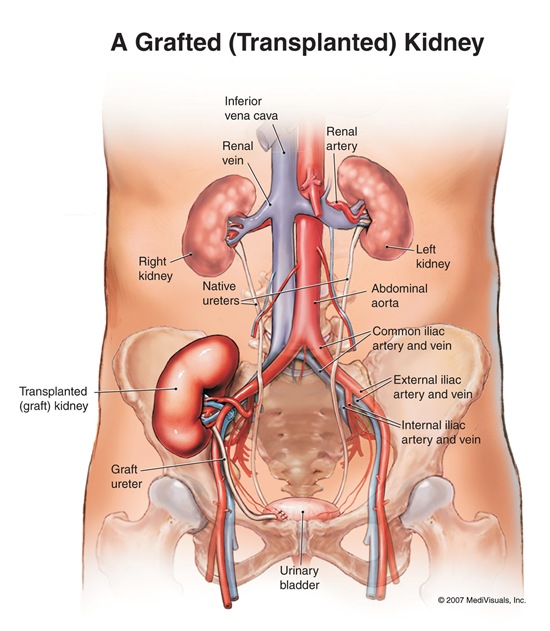
Surgery and Recovery
The surgery can take between 3-5 hours and can be done in two ways:
- Laparoscopy – the preferred method for kidney donor transplants.
- Open nephrectomy – done under general anesthesia and is more invasive.
What are the risks of surgery?
- Pain and you’ll receive medication
- Infection can delay healing and cause scarring or other problems. Treated with antibiotics.
- Pneumonia is an inflammation of the lungs caused by bacteria or a virus.
- Damage to the kidney the surgery could damage it.
- Blood clotting: make sure to move around after surgery to prevent them.
- Collapsed lung: the kidney is close to the lung and could be inadvertently opened during surgery.
- Urinary tract infection of the bladder or kidneys and will be treated with antibiotics.
- Allergic reaction to anesthesia.
- Death: the risk of death from surgery for living kidney donors’ is very low.



You must be logged in to post a comment.